📞  — free, 24/7
— free, 24/7
 — free, 24/7
— free, 24/7
| Dosage | Package | Price per Dose | Price | |
|---|---|---|---|---|
| 0.1/0.3% | 5 bottles | NZ$21.82 | NZ$145.47 NZ$109.10 Best Price Popular | |
| 0.1/0.3% | 4 bottles | NZ$26.09 | NZ$139.14 NZ$104.36 | |
| 0.1/0.3% | 3 bottles | NZ$32.40 | NZ$129.65 NZ$97.24 | |
| 0.1/0.3% | 2 bottles | NZ$43.89 | NZ$117.00 NZ$87.75 | |
| 0.1/0.3% | bottle | NZ$64.03 | NZ$85.37 NZ$64.03 |
Disclaimer: Tobradex is an eye medicine that may require a prescription depending on local rules. This page provides general information and is not a substitute for medical advice from a healthcare professional.
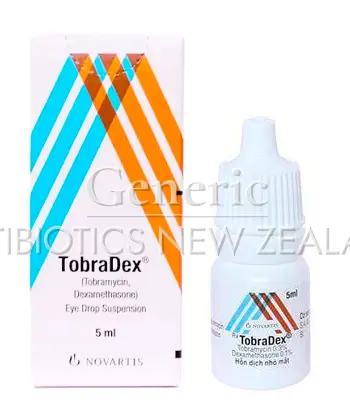
Tobradex is a medicine that combines two active ingredients: tobramycin, an antibiotic, and dexamethasone, a corticosteroid. The combination is designed to treat eye conditions where both infection-fighting and anti-inflammatory effects are helpful.
It is usually supplied as eye drops or a suspension that is applied to the surface of the eye. The drops are intended for use in the eye only, and the tip of the bottle should stay clean and away from the eye to avoid contamination.
In New Zealand, regulations about who may prescribe Tobradex can vary. A clinician or pharmacist can advise whether a prescription is needed in your situation. Always follow the local rules and the advice you receive from your healthcare professional.
Keep Tobradex in the original packaging with the cap closed when not in use. Do not share your eye medicine with others, and do not use it after the expiry date printed on the bottle. If the bottle or seal is damaged, do not use it.
If you have any doubts about whether Tobradex is suitable for you, ask your doctor or pharmacist for personalised guidance. They can check for allergies, other medical conditions, and whether this treatment is appropriate for your eye problem.
Tobradex is used to treat certain eye infections or inflammations where both an antibiotic and an anti-inflammatory are helpful. It is intended to reduce red, swollen, and irritated eyes caused by bacterial infections, under the supervision of a clinician.
It may be prescribed after eye surgery or after an eye injury to help prevent or treat infection and to reduce inflammation. Your clinician will decide whether Tobradex is appropriate for your recovery and how long you should use it.
The medicine can help relieve symptoms such as eye discharge, tenderness, and redness associated with the infection or inflammation. It is not a general remedy for all eye conditions, and treatment should be tailored to your specific diagnosis.
In some cases Tobradex is not suitable, such as when an infection is caused by viruses or fungi, unless your clinician says otherwise. Always use Tobradex exactly as prescribed and report any lack of improvement to your clinician promptly.
It is intended for ocular use only. Do not apply Tobradex to other parts of the body or swallow it. If you notice any new symptoms after starting treatment, contact your clinician for advice.
The two components work in different ways. Tobramycin is an antibiotic that fights certain bacteria that can cause eye infections. Dexamethasone is a corticosteroid that reduces inflammation and swelling in the eye.
By combining these actions, Tobradex aims to clear infection while limiting inflammatory symptoms that contribute to discomfort and slower healing. The result can be faster relief of irritation and improved vision when used as directed.
Because it is a steroid-containing eye drop, Tobradex can sometimes affect eye pressure or healing if used for a long time. Your clinician will monitor you if longer treatment is needed, and you should report any eye changes or new symptoms promptly.
Like all medicines, Tobradex may have more benefit in some people than others. If you do not notice improvement within a few days, or if symptoms worsen, seek medical advice. Do not extend treatment beyond what your clinician has recommended without checking first.
In New Zealand, safe use also means noting any potential interactions with other eye drops or systemic medicines. Always tell your healthcare professional about all medicines you are taking so they can advise you appropriately.
Before using Tobradex, wash your hands well with soap and water. Dry them completely before handling the bottle or touching your eyes.
If you are using a suspension, gently shake the bottle as directed by the label or your clinician to ensure the medication is evenly mixed. Do not use if the solution appears clearly separate or discoloured.
To apply the drops, tilt your head back and pull the lower eyelid down to form a small pocket. Look up and gently squeeze one drop into the pocket, taking care not to touch the dropper tip to your eye or eyelashes. After releasing the eyelid, close your eye for a moment and blink slowly to spread the drop over the surface.
If you are using Tobradex in both eyes, repeat the procedure for the other eye with a clean dropper. If you are using other eye medicines, wait a few minutes between different drops unless your clinician instructs otherwise.
Avoid wearing contact lenses while using Tobradex unless your clinician has advised that it is safe to do so. If you wear lenses, remove them before applying the drops and reinsert them only after the recommended waiting period, as advised by your clinician. Store and handle the bottle as instructed on the label or by your pharmacist.
Do not use Tobradex if you have a known allergy to tobramycin, dexamethasone, any other aminoglycoside antibiotics, or any ingredient in the product. If you notice signs of an allergic reaction such as swelling or severe itching around the eye, stop using Tobradex and seek medical help.
People with a fungal eye infection or certain viral eye infections should not use Tobradex unless advised by a clinician, as steroids can worsen some infections. Your clinician can assess whether Tobradex is appropriate for your condition.
If you have a history of glaucoma, increased eye pressure, or long-term use of steroid eye drops, inform your clinician before starting Tobradex. Steroids can affect eye pressure and healing, so ongoing monitoring may be required.
If you are considering Tobradex for a child, or if a child is already using it, speak with a healthcare professional about appropriate dosing, safety, and monitoring. The suitability can differ from adults.
If you wear contact lenses, you should discuss with your clinician whether Tobradex is suitable for you and for how long you should avoid wearing lenses during treatment.
Short-term use of Tobradex under medical supervision is common, but long-term or excessive use can increase the risk of side effects such as increased eye pressure, cataract formation, or delayed healing. Your clinician may check your eye pressure if you require extended therapy.
Treatment with steroids can mask symptoms of worsening infections. If symptoms persist or worsen after a few days of treatment, contact your clinician promptly for reassessment. Do not extend the course of treatment without advice.
There is a potential for minor systemic absorption through the eyes, which is usually small, but it may be relevant for people with certain medical conditions. Discuss any concerns with your clinician, especially if you have kidney problems or are taking other medicines.
If you experience blurred vision, eye pain, severe redness, discharge, or signs of an allergic reaction, seek medical help urgently. Do not drive or operate machinery if your vision is affected until it clears.
Storing Tobradex properly helps maintain its effectiveness. Keep it at room temperature, away from heat and sunlight, and keep it out of reach of children. Do not use after the expiry date printed on the bottle or if the packaging has been damaged.
Common side effects may include temporary burning, stinging, or blurred vision just after applying the drops. Some people may notice increased tearing or mild eye irritation that settles with continued use.
Less commonly, people may experience a changed or metallic taste, dry eyes, or discomfort when blinking. These effects are usually temporary and resolve after stopping or adjusting treatment as advised by your clinician.
More serious but rare effects can include a worsening of infection, eye swelling, or eye pain, as well as symptoms of an allergic reaction such as rash, itching, or swelling of the face or lips. If you notice any of these, seek medical help promptly.
Because Tobradex contains a steroid, there is a potential risk of increased intraocular pressure with prolonged use. If you have a history of glaucoma or eye pressure issues, your clinician will monitor you and adjust treatment if needed.
If you experience persistent vision changes or any persistent symptoms that worry you, contact your clinician for advice rather than continuing treatment on your own.
Tell your clinician about all eye medicines you are using, including over-the-counter products and any eye drops prescribed by other providers. Interactions can occur with other antibiotic or steroid eye drops, especially those that share similar active ingredients.
Do not use Tobradex together with other ophthalmic products unless advised by your clinician. This includes solutions for contact lenses and products you apply to the eye for irritation or allergy.
If you are using oral medicines or systemic steroids, discuss with your clinician because combined steroid exposure can increase certain side effects. Your clinician can plan a safe treatment approach for you.
If you notice a change in how another medicine feels or works after starting Tobradex, tell your clinician. They can determine whether a different regimen is needed.
Storage and handling practices matter for interactions too. For example, avoid sharing eye drops with others and keep the bottle closed when not in use to preserve its integrity and reduce the risk of contamination.
The safety of Tobradex in pregnancy and breastfeeding has not been fully established. It should be used only if the potential benefits justify any potential risk to the fetus or infant, and under the guidance of a clinician.
If you are pregnant or planning to become pregnant, or if you are breastfeeding, tell your clinician before starting Tobradex. They can help weigh the benefits against potential risks and discuss alternatives if needed.
If you become pregnant while using Tobradex, contact your clinician promptly. Do not discontinue treatment without advice, unless you are told to stop for safety reasons.
As with many medicines, the advice may differ based on individual circumstances. Always seek personalized guidance from your healthcare professional in New Zealand.
In all cases, use Tobradex only as prescribed and monitor for any unusual symptoms in both you and your baby if you are breastfeeding. Your clinician can provide the best guidance for your situation.
Many people notice an improvement in symptoms within a few days, but this varies depending on the infection and inflammation being treated. If there is no improvement after several days, contact your clinician for advice.
If you miss a dose, apply Tobradex as soon as you remember, unless it is almost time for your next scheduled dose. Do not double the dose to catch up. If you are unsure, contact your clinician for instructions.
Yes, often it can be used with other eye drops, but you should space them out by several minutes. Always follow your clinician’s instructions about the order and timing of multiple eye treatments.
Contact your clinician if you notice no improvement within a few days, if symptoms worsen, if you experience severe eye pain, vision changes, or signs of an allergic reaction. Seek urgent medical help if you have sudden severe symptoms.
Use during pregnancy or breastfeeding should be decided by a clinician after weighing benefits and potential risks. Do not start or continue treatment without medical advice.
Use in children should be supervised by a clinician. The safety and appropriate dosing can differ from adults, and a child’s clinician will provide guidance tailored to the child’s age and condition.
If you develop swelling of the face, lips, tongue, or throat, severe itching, or a skin rash, seek medical help urgently. Do not continue using Tobradex until advised by a clinician.
Commonly reported effects include temporary burning, stinging, or blurred vision right after applying the drops. Some people may notice tearing or mild eye irritation that improves with use.
Yes, you may experience temporary blurred vision or light sensitivity after instillation. If vision remains blurred for longer than a short period, avoid driving or using heavy machinery until vision clears, and seek advice from your clinician.
Store Tobradex as instructed on the label, away from heat and direct light. Keep the bottle capped when not in use and out of reach of children. Do not use beyond the expiry date or if the bottle appears damaged.
This information reflects common clinical practice for ophthalmic combinations similar to Tobradex and aligns with general patient information provided by healthcare professionals in New Zealand. Always refer to the official patient information leaflet supplied with Tobradex and consult a healthcare professional for personalised advice.
Official leaflet or product packaging provided by the manufacturer is the primary source for device-specific details, including any warnings, precautions, and dosing instructions. Your local pharmacist or doctor can help interpret these details in the context of your health status.
Medicines regulatory guidance and pharmacy practice standards in New Zealand emphasize consulting a clinician for prescription requirements and for questions about safety, interactions, and use during pregnancy or breastfeeding. If you have questions about Tobradex in your region, ask your pharmacist or doctor for the most current information applicable to you.
14–21 days. Free from NZ$341.82 .
5–9 days. NZ$51.27
−10% when paying with cryptocurrency.
−10% on all repeat orders.
All orders are packed in neutral, unbranded boxes with no product name on the outside.
